Newborn Resuscitation
Improving resuscitation at delivery of newborns 35 weeks and greater in Oregon.
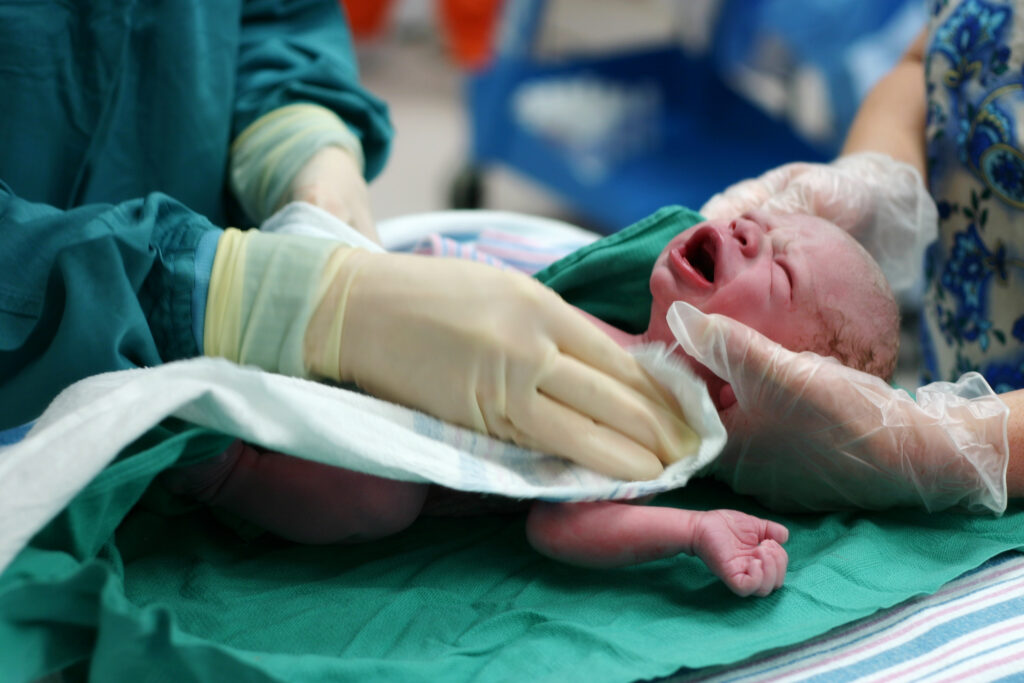

Background
Newborn resuscitation is a critically important, but low incidence intervention that can be frightening, stressful and sometimes traumatizing to parents, family members and clinicians. Effective systems along with regular training, drills and simulation are needed to keep resuscitation teams prepared for both clinical and communication aspects of high quality care. An Oregon Perinatal Collaborative workgroup created toolkits and resources for hospital teams and community birth settings with content organized to support teams in addressing key aspects of systems and care.
We are excited to share that multidisciplinary hospital and community birth teams across the state are working together on implementation of the Oregon toolkit from September 2025-September 2026 to improve newborn resuscitation through a quality improvement initiative that includes virtual and in person meetings, as well as onsite simulation support. This initiative focuses specifically on decreasing morbidity and mortality among newborns greater than or equal to 35 weeks.
Additional Resources
Clicking on each tab on the left below will display the additional content and links for each section
Key readiness takeaway: Readiness for newborn resuscitation requires a clearly identified and skilled team with both clinical and communication expertise.
Key timely intervention takeaway: Close adherence to the NRP algorithm can lead a trained team through timely and effective evaluation and resuscitation of a newborn and improve outcomes.
Additional resources and information will be added here as they are created / available.
Key post resuscitation care takeaway: Timely stabilization and/or transfer of ill newborns can improve outcomes.
| Neonatal Transfer SBAR |
| Post Resuscitation Care Table |
Key communication takeaway: Effective communication ensures team preparation and performance and improves patient safety as well as parent/family experience of care.
| Debrief Example 1 |
| Debrief Example 2 |
Key systems learning takeaway: Consistent case review of newborn resuscitation events can improve patient safety and quality of care when areas for improvement are identified and acted on and learning is shared with all members of resuscitation teams / community midwives.
| Newborn Resuscitation Chart Review Template |
In March 2025 the Oregon Perinatal Collaborative conducted a focus group on newborn resuscitation. The focus group was for parents of a child who: was born in Oregon in a hospital, freestanding birth center, or home birth within the past 3 years; was resuscitated at birth; and was discharged from the NICU within 14 days of birth (if admitted to the NICU).
The definitions below are provided to ensure consistency in use by teams with active quality improvement work throughout the OPC initiative. There are additional definitions/ specifications provided for data/measures in a separate document for teams participating in the quality improvement initiative.
Alternative Airway: Devices used to support or provide ventilation, including laryngeal mask, supraglottic airways, and endotracheal tubes (ETT).
Drills: Practice of individual skills or portions of newborn resuscitation with individual or subset of the team.
Newborn Resuscitation: The use of Positive Pressure Ventilation (PPV) with or without the use of an advanced airway, chest compressions, or medications to treat a newborn who does not breathe after birth despite appropriate initial actions as outlined in NRP.
Pre-Brief: The action of the delivery/resuscitation team verbally providing and receiving precise and essential information to plan for a potential resuscitation.
Respiratory Support: Support provided to newborns at birth who are not breathing or require support for labored breathing. This can include CPAP, PPV and intubation.
Simulation: Multidisciplinary (all members of resuscitation team), team-based practice of newborn resuscitation that includes pre-briefing, resuscitation, and debriefing using a realistic preplanned clinical case that allows multiple aspects of the care to be practiced (technical skills, equipment, team communication, EHR, telehealth, etc). Can occur in a simulation lab or on the unit (in situ) and include low or high- fidelity newborn model.
Content Last Updated: September 11, 2025
